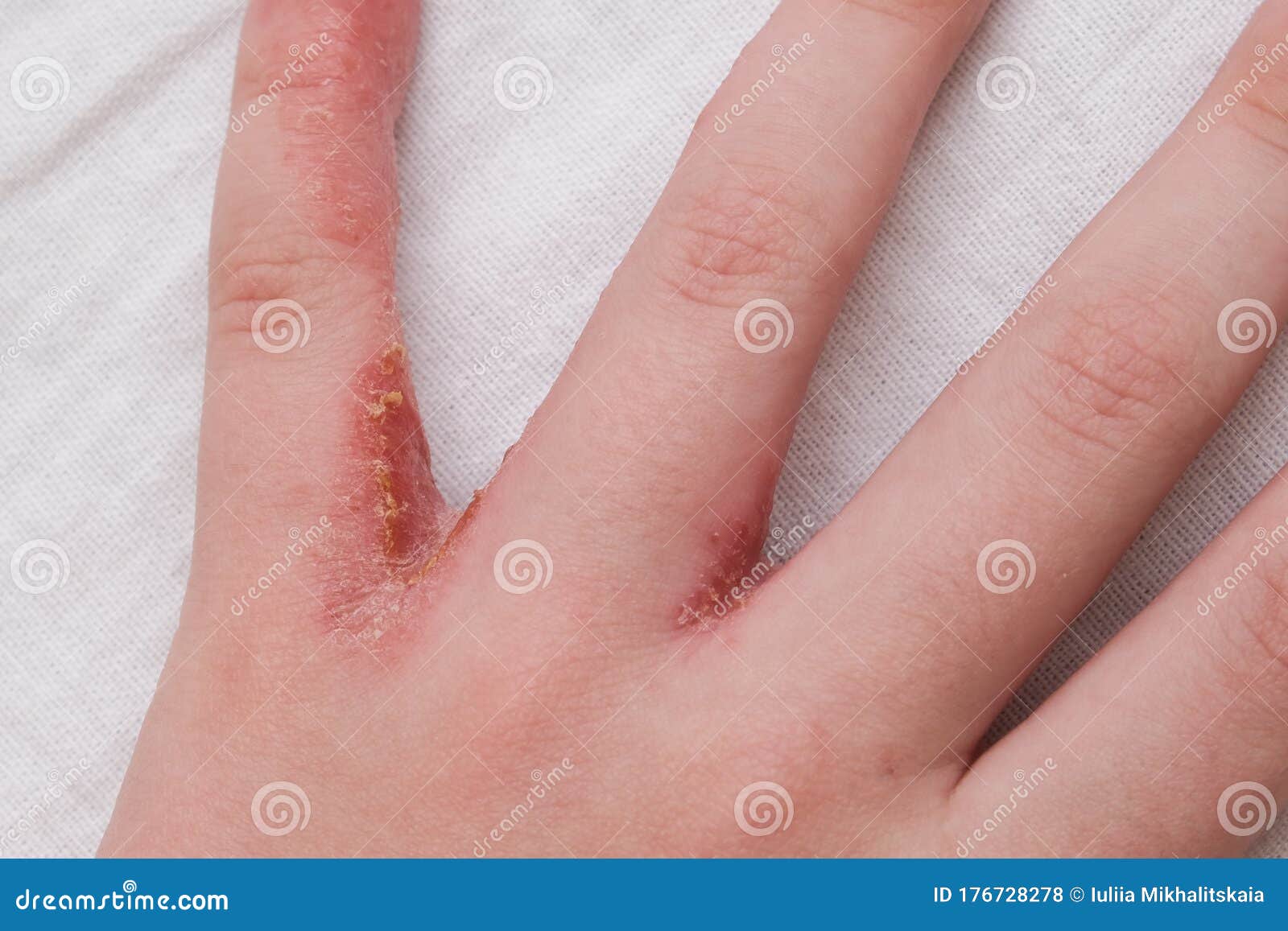
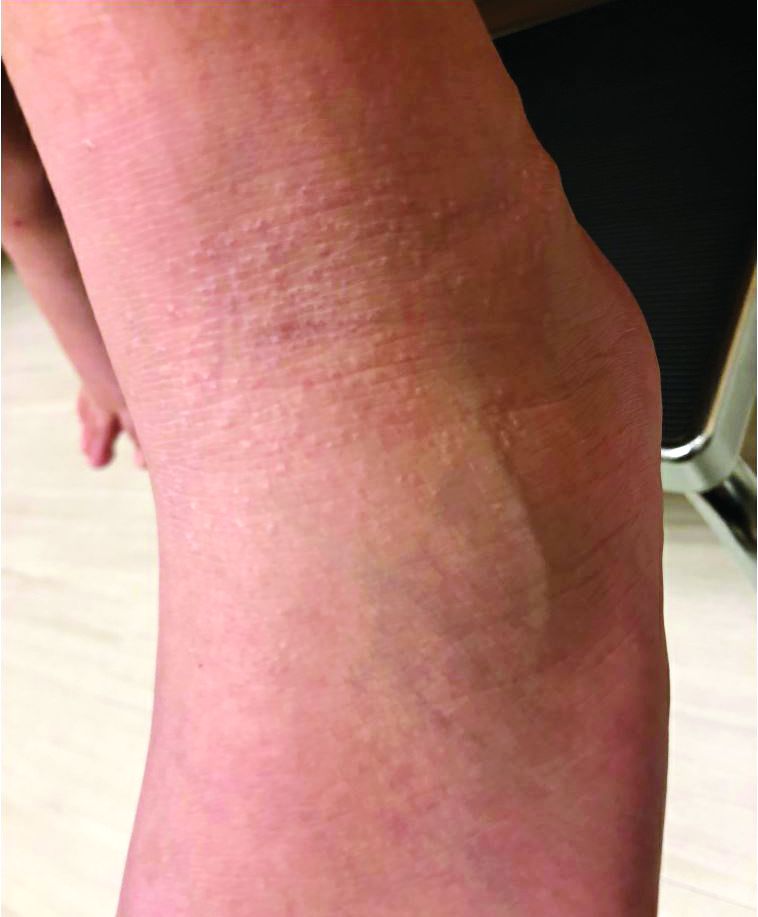
Picture B and C: Examples of mucosal involment of oral cavity Picture A: Target lesion, note central duskiness 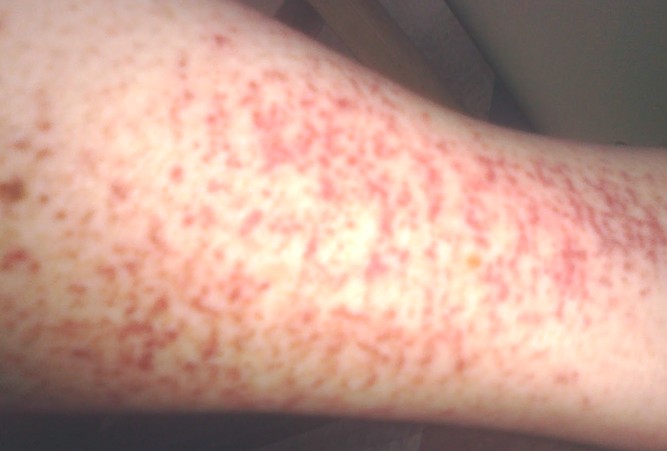
Treatment is largely supportive care and discontinuing offending drug agents. The etiology of SJS may be drug related (ie: anti-epileptics, NSAIDS, sulfonamides, acetaminophen) or infectious (ie: HSV, mycoplasma, EBV) or. Universally, hemorrhagic crusting of the lips and oral cavity are seen with SJS. Those that appear ill, infants 2 mucosal sites, i.e. Those with lesions proximal to the eyes should be urgently evaluated by ophthalmology. Usually treatment options with acyclovir, valacyclovir or famciclovir are most efficacious when given within 48 hours of symptoms. In a child with atopic dermatitis with an overlying herpetic rash is referred to as eczema herpeticum. If an HSV rash is located on the digits, it is referred to as a herpetic whitlow. This differs from herpangina, which commonly appears on the soft palate, tonsillar pillars, uvula and posterior pharynx (see below for description). HSV-2 infection is commonly associated with genital infections and typically transmitted through sexual contact.Ī child with herpetic gingivostomatitis usually has a fever accompanied by a vesicular and/or ulcerative rash of the buccal mucosa, tongue, gingivae, and perioral skin. HSV-1 infection typically causes a localized infection of the mouth (herpetic gingivostomatitis), lips and/or eyes. The classic rash associated with HSV is a painful vesicular (1-2 mm) and/ or ulcerative rash on an erythematous base. Herpes Simplex Viral (HSV) Infection can cause localized or widespread infection. Diagnosis is largely a clinical diagnosis as the bullae are sterile. SSSS is typically associated with a positive Nikolsky sign, rubbing of the skin that causes skin desquamation or creates abullae within minutes. Children less than 5 years are usually affected and present with a generalized tender erythroderma and flaccid bullae. SSSS is a toxin mediated rash produced by Staphylococcus aureus. Pictures from Staphylococcal Scalded Skin Syndrome (SSSS) Confirmatory tests include culture of the blood and CSF. Late cutaneous features will include purpuric (non-blanching) lesions with jagged edges. Early on the rash may appear morbilliform or urticarial macules and papules that often progress to petechial, pustules and vesicles. Apart from fever, irritability and meningitis signs and symptoms, 2/3 of those affected will have a cutaneous manifestation. Children less than 12 months are at the highest risk of meningococcemia. Meningococcemia, which is due to Neisseria meningitides, will often present in an ill appearing patient. Below is a table that outlines the descriptions of rashes.ĭifferential Diagnosis Infectious Rashes in Ill Appearing Child When assessing the rash, describing the appearance, distribution and associated symptoms are paramount in figuring out the etiology of the rash. The quality of central pulses (brachial, femoral, carotid) is also paramount in the circulation assessment. When assessing the child’s circulation, the clinician needs to be aware whether the heart rate and blood pressure are age appropriate. The child’s breathing should be assessed including the oxygen saturation and respiratory effort. Urticaria may be associated with airway compromise such as stridor in the case of anaphylaxis. In the initial evaluation, the child’s airway should be assessed. By going through the ABC’s as well as understanding age appropriate vital signs, the clinician should be able to identify children that are ill and may require a work up or a timely intervention. The general approach to the evaluation of rashes is to first identify whether the child is sick versus not sick. Rash is a common chief complaint for children in the emergency department.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
